#WorldDiabetesDay – Nurses make the difference
14 Nov 2020
This world diabetes day, as well as raising awareness of diabetes, we should be celebrating the contribution our nursing colleagues make to the lives of people with diabetes.
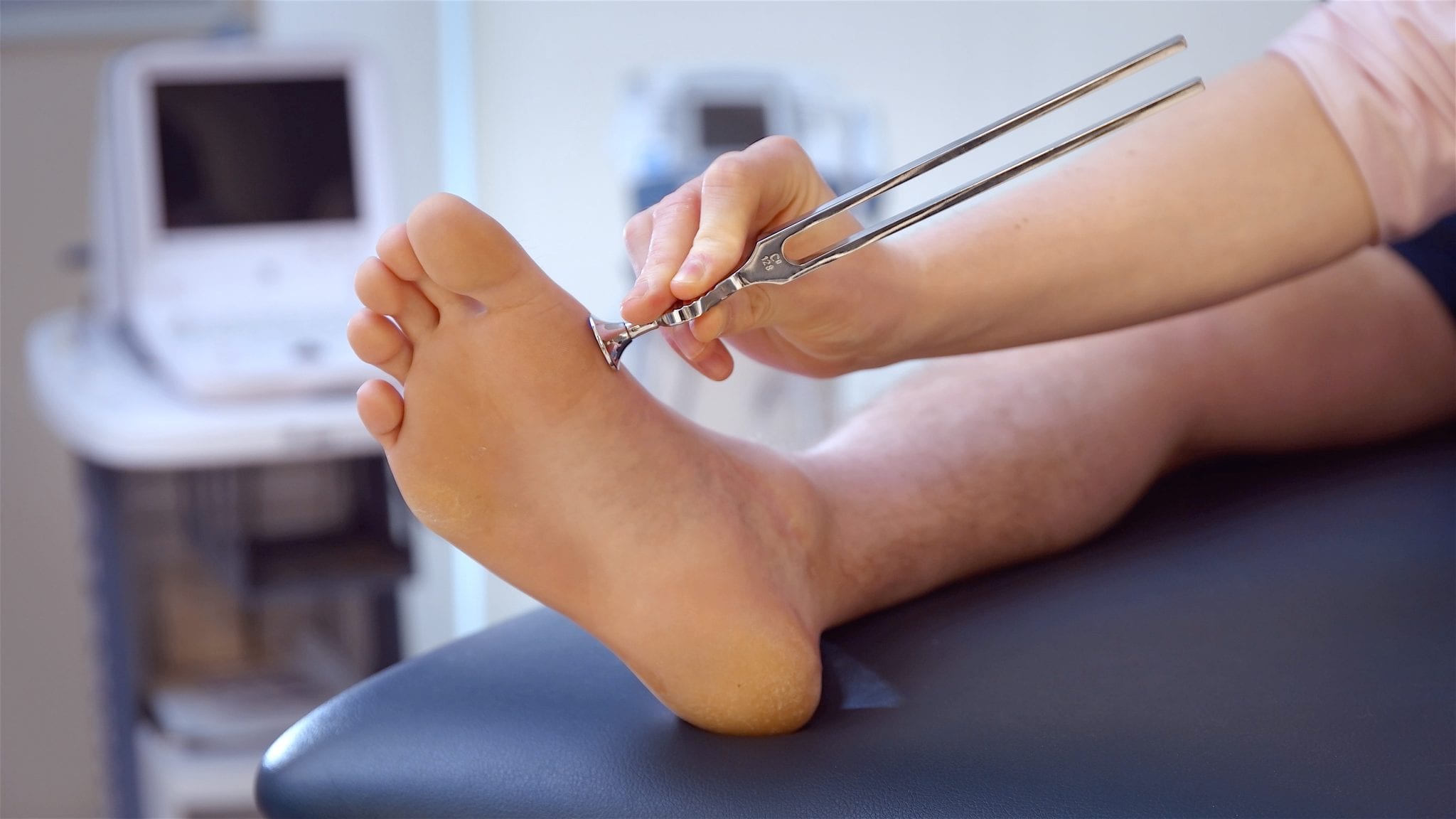
To mark #WorldDiabetesDay today, we’re delighted to be able to publish this guest blog by Matthew Collison from our Faculty of Podiatric Medicine, on the role of nursing staff in providing first class patient care to patients with diabetes.
World diabetes day is held annually on the 14th November, the birthday of Sir Frederick Banting, who co-discovered insulin with Charles Best in Toronto in 1922. The day was initiated in 2006 by the World Health Organisation (WHO) and the International Diabetes Foundation (IDF) to build awareness of the growing health threat diabetes poses globally. This year, for world diabetes day, the theme is “Nurses make the difference.” This is to shine a light on the role that nurses play in the care of people with diabetes.
Globally, there are approximately 425 million people with diabetes according to the WHO. While not all of us are involved in the management of diabetes, every healthcare professional will encounter patients with diabetes in their daily practice. As a podiatrist, much of my training had been dedicated to the diabetic foot, however as I have progressed in my career, my interest moved towards musculoskeletal podiatry and away from the diabetic foot. That was, until the COVID-19 pandemic struck, and I found myself redeployed to the community diabetic foot team.
Nurses make the difference
A multidisciplinary approach to managing diabetes is essential in optimal management. Nurses are key to this, and are involved at every point of the diagnosis, management and prevention of diabetes and its complications. Data from the WHO suggests that there is a global shortage of nurses of around 5.9 million, with the greatest shortfall in low- and middle-income countries. Low-and middle-income countries are also experiencing the greatest increase in new diabetes diagnoses.
For many with diabetes, nurses will be the first port of call and the main contact in the management of their diabetes. On diagnosis, many patients will have education from nurses through DAFNE and DESMOND and similar courses. They may have their condition monitored and managed by diabetes specialist nurses, or by the practice nurse. They may have their insulin administered at home by the district nurse. They should have their feet checked annually by the practice nurse or by an assistant practitioner such as a healthcare assistant or nursing associate. When things go wrong, they may see the district and tissue viability nurses for wound care, as well as the rest of the multidisciplinary team. For many patients, the nurse becomes a familiar face, with whom they can discuss not only their care but also increasingly discuss social and mental health needs. Nurses often take a signposting role, ensuring access to other professions and medical specialties.
COVID-19
COVID-19 of course has changed the model of care for many with diabetes, however nurses remain at the forefront of the management of diabetes. What the pandemic has done is that it has hastened the adoption of technology to modernise diabetes care. Many educational programmes and sessions are now delivered online, meaning that patients can continue to access this invaluable information in the safety of their home. Diabetes nursing reviews are increasingly being delivered by telephone and virtual platforms. There is of course, the continued need for face to face nursing care.
During lockdown, where many with diabetes were advised to shield, visits from district nurses were some of the only contact for our most vulnerable patients. As part of my redeployment, I took on some of the district nurses woundcare caseload in addition to the high-risk podiatry cases. I was struck by the social isolation experienced by some of the patients and saw the difference that the contact from the district nurses made to their wellbeing. To them, the nurses were a lifeline. I also reviewed patients on joint visits with the community tissue viability nurses, and I was impressed by their skill and knowledge. For patients with diabetes, nurses do make the difference.
Challenges in the UK and Globally
It is well known that there is a shortage of healthcare professionals in the UK. This is across the board including nurses, doctors, and allied health professionals. The government has set a target of 50,000 new nurses by 2025. This will be a monumental task, especially given the reduction in applications for university places in nursing and the relatively high attrition rate amongst nursing students. There is a known shortage of diabetes specialist nurses, and of district nurses. With the prevalence of diabetes on the increase, without urgent action there is likely to be a significant gap in care for patients with diabetes.
The picture globally is similar. There are shortages of qualified nurses of 5.9 million internationally, however the shortage is greatest in low- and middle-income countries. With around two thirds of newly diagnosed cases of diabetes being in these low- and middle-income countries, without significant investment, healthcare systems will be unable to meet this increased demand for care.
Get involved
This world diabetes day, as well as raising awareness of diabetes, we should be celebrating the contribution our nursing colleagues make to the lives of people with diabetes. The IDF held a twitter chat on the role of nurses in diabetes @IntDiabetesFed on Friday 13th November. Lockdown may limit in-person events to mark the day, but you could always reach out to colleagues virtually. If you are feeling active, you could virtually take part in the Global Diabetes Walk to raise funds and awareness https://www.worlddiabetesfoundation.org/global-diabetes-walk-2020.
Make sure you share your WDD exploits on social media by sharing stories of great care in diabetes, of inspirational colleagues, and tips for those with diabetes with the hashtags #WDD, #WorldDiabetesDay and #NursesMakeTheDifference. There is a WDD app to take your ‘blue circle’ selfies for your social media accounts, and make sure to tag the college @rcpsglasgow and @WDD on twitter and Instagram.
Latest news and statements
Key priority areas
Topics
- Workforce
- Wellbeing
- Equality, Diversity and Inclusion
- Climate Change
- Health Inequalities
- College
- Obesity
- COVID-19
Archive
Key links
Tweets by @rcpsglasgow